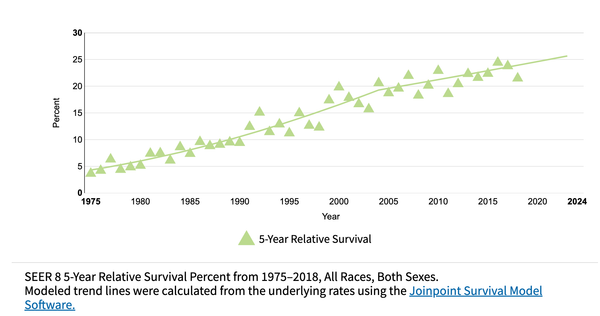
Esophageal adenocarcinoma incidence increases in Netherlands
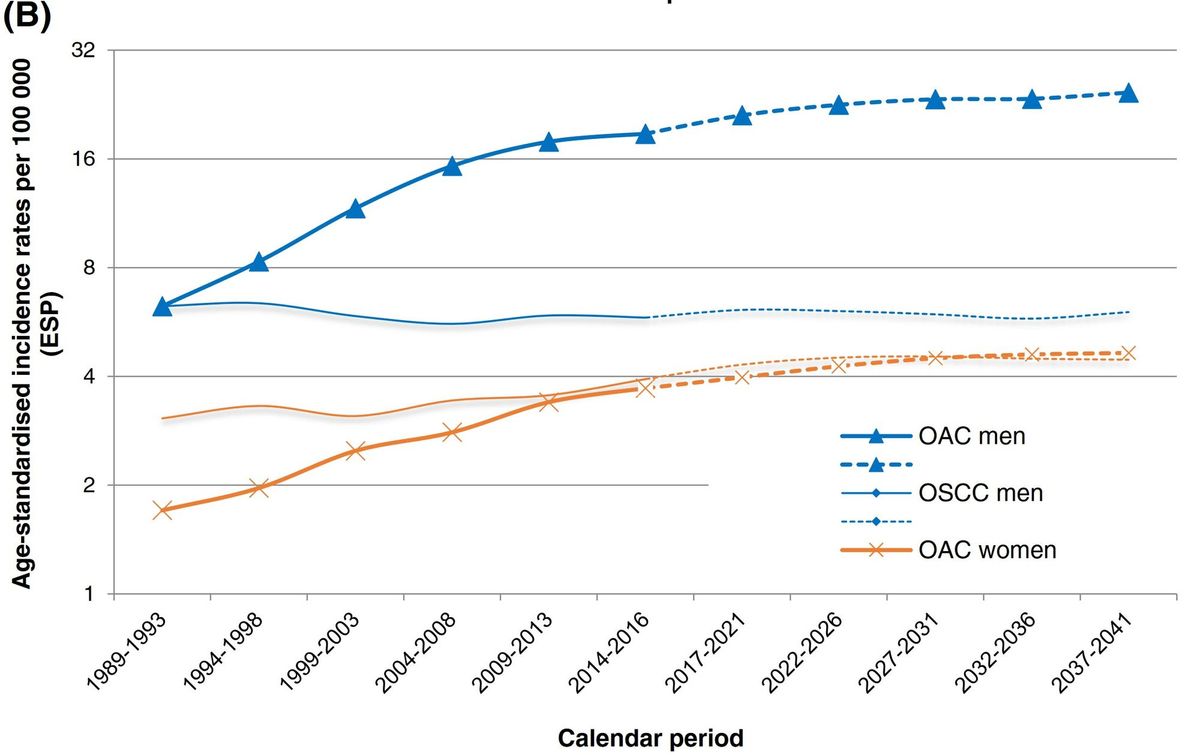
The authors calculated temporal trends in esophageal adenocarcinoma from 1989-2016 in the Netherlands, finding substantial increases. They projected rates about 30% higher in the late 2030's.
Int J Cancer. 2022 Feb 1;150(3):420-430. doi: 10.1002/ijc.33836. Epub 2021 Oct 16.
Trends and projections in the incidence of oesophageal cancer in the Netherlands: An age-period-cohort analysis from 1989 to 2041
Femmie de Vegt, Jessie J J Gommers, Hans Groenewoud, Peter D Siersema, André L M Verbeek, Yonne Peters, Mireille J M Broeders
Abstract
In Western populations, the incidence of oesophageal squamous cell carcinoma (OSCC) has been declining, whereas the incidence of oesophageal adenocarcinoma (OAC) has been increasing. Our study examines temporal trends in the incidence of oesophageal cancer in the Netherlands between 1989 and 2016, in addition to predicting future trends through 2041. Data from the Netherlands Cancer Registry and Statistics Netherlands were collected to obtain incidence trends of OSCC and OAC for the period 1989 to 2016. Age-period-cohort (APC) modelling was used to estimate the contribution of age, calendar period and birth cohort on the observed incidence trends. To predict the future numbers of new cases of both OSCC and OAC from 2017 to 2041, log-linear APC models were fitted to the trends of 1989 to 2016. The age-standardised incidence rates of OSCC have decreased slightly for men and increased slightly for women. In contrast, a marked increase in the incidence of OAC was observed, ranging from 2.8 per 100 000 persons in 1989 to 10.1 in 2016. This increase in OAC incidence was more prominent in men, and it will result in an increased risk of OAC for successive generations. Future projections indicate that the incidence of OAC will further increase to 13.1 per 100 000 persons in 2037 to 2041, meaning that there will be 13 259 cases of OAC in 2037 to 2041, as compared to 9386 diagnoses in 2017 to 2021. The changing epidemiologic trends in oesophageal cancer in the Netherlands should be reflected in the development of prevention, early detection and treatment strategies.
PMID: 34605022 DOI: 10.1002/ijc.33836